There is something so sweet about feeding a baby. The way they eagerly suck down the milk and then slowly drift off to sleep towards the end of a feeding. Seems simple enough, right? All babies love to snuggle and eat – or at least that’s what I thought before I became a mom myself.
First Feeding
Two weeks into motherhood I sat in a hospital rocking chair happily anticipating feeding my son for the first time. He had been using a feeding tube for the better part of a week while recovering from open-heart surgery. The speech pathologist was there evaluating him and handed me a tiny bottle with 10MLs of milk in the bottom of it. I must have looked at her like she was nuts. Ten MLs? One-third of an ounce? Are these people ever going to let my kid just eat like a normal baby?? This kid is hungry!
I put the bottle up to his lips and he quickly pressed them closed. Hmm. After a few minutes of coaxing and repositioning he took three perfect little sips and fell back to sleep.

He drank only 5MLs at that feeding and proceeded to do exactly the same routine for every feeding for a week. This “simple” feeding routine was going to be a little harder than I anticipated.
Milk Strike
The medical staff encouraged me that after his next heart surgery he would have much more energy and eating would be easier. He did eventually take more milk at each feeding, but we still had to supplement by putting additional milk through the feeding tube daily. His second surgery came and went very successfully. I was so excited to see Calvin eat better and ditch the feeding tube! But, Calvin had other plans. After his surgery he completely stopped eating my mouth. He would not allow one drop of milk to pass his lips. I was devastated.
All in Good Time
The doctors told me he would eventually eat in his own time. I felt like a mom failure though. How could I not do something as simple as get my baby to eat? I followed all of their advice to a T but Calvin would not budge. Finally someone mentioned feeding therapy. I had no clue that was an option for us. I had heard of feeding therapy for swallowing disorders but didn’t know it could be beneficial when your baby just downright refused to eat. YES!! Let’s do some feeding therapy!
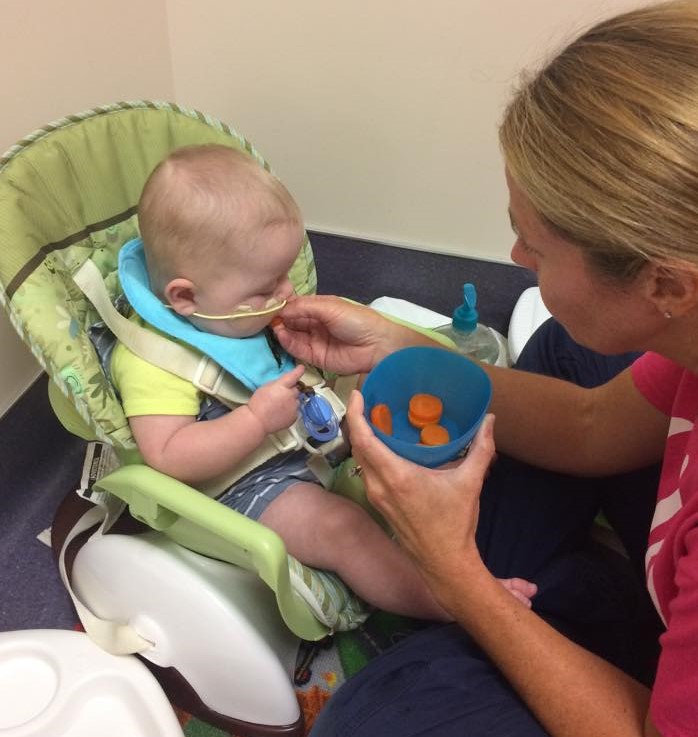
At 5 months old, Calvin went to his first feeding therapy appointment and it was a breath of fresh air. For the first time in 5 months I felt like someone was listening to me and seeing the problem. Calvin’s doctors were wonderful, but they were concerned about good heart function and healthy weight gain. Calvin’s feeding therapist understood that weaning from the feeding tube was a quality of life issue for us. She was in my corner and gave me the tools and encouragement I needed to help Calvin eat.
Calvin began therapy nearly 100% tube dependent. After 4 months of weekly visits, and lots of practice at home, he discharged from feeding therapy and never used a feeding tube again. Victory!
Practical Tips for feeding
Below are our therapist’s best tips for fostering a normal eating environment and encouraging good oral experiences. I hope you find these nuggets of her advice as helpful as I did. If you are currently struggling with oral feeding at home I would encourage you to consider these strategies and seek the help of a Speech-Language Pathologist who is experienced in working with children with feeding difficulties.
Check out the tips below.
Ideas for Mealtimes
Eating is not a simple process, it requires food be ingested, swallowed and finally digested. Disruption of any of these processes may lead to malnutrition, poor growth, delayed development, and loss of general health and well-being. Here are some tips to try with your child at home to make mealtimes less stressful. If you have tried many of these things and you’re continuing to struggle, know that feeding therapy is available and is designed to help with food refusals, food selectivity by type or texture, dysphagia (swallowing difficulty), oral motor dysfunction, recurrent vomiting, failure to thrive, mealtime tantrums, and feeding tube dependence. You can download these tips as a pdf here.
To promote regular hunger cycles and increase intake:
- Place your child on a regular feeding schedule
- Limit meals to 20-30 minutes
- Do not allow grazing on liquid or food between meals
- Position child in a supportive seating system for all meals and snacks
To encourage cooperation during meals and acceptance of food:
- Never force-feed or sneak bites into mouth when it’s open to laugh, cry…
- Keep mealtime interactions fun and pleasant for your child
- Avoid cleaning face and hands during meals as this can be averse to children with feeding difficulties
- Give lots of praise and attention for desired actions (e.g. touching foods, trying to self feed, taking a bite)
- Use positive statements, not questions (e.g. Say “food stays on the table”, “your turn”, “you do it”, “it’s bumpy and white!” instead of, “no throwing”, “do you want more?”, “can you do it?”, “Please?”)
To promote calmly sitting during mealtime:
- Consider sitting your child in a chair for play. Use toys; as tolerance increases, incorporate utensils, bowls, cups and food
- Set a time limit for sitting, begin with a short period (e.g. 3 minutes) and increase to 20-30 minutes
To facilitate improved oral intake over tube feedings:
- Place on bolus feeds as much as possible
- Consider giving bolus feeds over 20-30 minutes
- Provide your child with positive oral experiences with pleasurable touch, teethers, and empty utensils
- Continue to provide as normal a feeding environment as possible during bolus feeds
- Position the same way you would feed orally (in high chair)
- Place the pump or tube behind them, out of view
- Sit and interact with them as if they were eating orally
- Feed in the same location as you would orally (in kitchen or dining room)
- Provide oral stimulation and food/smell/taste/experiences as tolerated, in order to teach the association between satiety and food experiences
Remember:
Use lots of praise when your child takes a bite, touches a new food, or puts it in their mouth. Try not to give attention to those behaviors we do not want continued, such as turning away or pushing food away.
Encourage your child to participate in mealtime preparation (cooking, serving family members) to provide food education and sensory information regarding non-preferred food items.
Please address issues regarding constipation, reflux, oral hygiene and thickening of liquids with your child’s medical team as these are issues which may impact oral feeding.
Feel free to contact our team with any questions or concerns. These suggestions are offered as general guidelines, please contact your medical team with specific concerns.
301 High Hopes Court
Franklin, TN 37064
615-661-5437
Linda Tyson, MA, CCC-SLP
Lori Scott, MS, CCC-SLP, CLC
Download PDF of Ideas for Mealtimes
Also read my blog on questions you may have now that you are home from the hospital.


